12-24 Months, Augma Bone Cement Academy, Bone Cement Expert, Clinical Cases, Clinical Indication, Clinician, Dental Notation, Images, Lower Left Molar, Media, Peri-Implantitis, Post-Op Period, Ridge Preservation
About a Peri-Implantitis
The patient is a young retiree who practices good oral hygiene and does not smoke. Tooth #36 (19) was replaced with an implant 16 years ago, and #37 (18) was replaced 8 years ago. He returned for an unscrewing of the crown of #37 (18), which induced an occlusal trauma. This ultimately led to peri-implantitis trauma, and mobility of the implant due to peripheral bone loss.
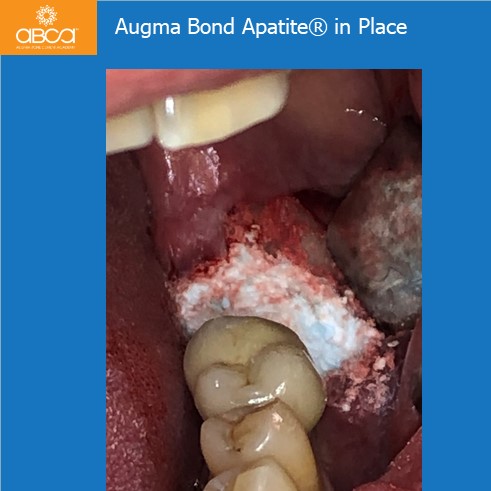
Due to the proximity to #36 (19), I chose to remove #37 (18), and to graft. The height of the bone over the mandibular nerve is low, so I decided to perform a GBR with Biphasic Calcium Sulfate (Augma Bond Apatite®, 1 syringe), while deposing the implant in order to maintain bone level and regain bone loss. Any other technique which required a membrane to stabilize and protect the graft material would have been difficult to use in this sector.
After 13 months, I proceeded to place the implant into true, new bone. (Surcam, S-type, 5×11.5). Blood supply to the area was satisfactory and the bone was D2-D3.

About a Peri-Implantitis. Clinical case by Dr. Stephane Berg, DDS